Theme: Scrutinizing the Emergence, Control and Public Health of Neglected Diseases
Tropical Diseases 2018
We are hereby pleased to invite all the participants from all over the world to attend the “Neglected Tropical Diseases Congress: The Future Challenges” which is going to be held on December 5-6, 2018 at Dubai, UAE. The conference includes prompt presentations, special sessions, workshops, symposium, oral talks, poster presentations and exhibitions. We expect your kind presence at the conference which will discuss the recent emerging diseases, outbreaks, categories, epidemiology, diagnosis, therapeutics etc.The Theme of the conference is "Scrutinizing the Emergence, Control and Public Health of Neglected Diseases".
Why to attend?
Neglected Tropical diseases 2018 provide a worldwide platform and recognition to an analyst who enlightens the advanced and unique methods in Infectious Diseases. Dynamic speakers, improvements, and most updated information are particular components of this gathering and personalities from all across the globe focusing on finding out about recent emerging disorders. An expanding number of distinguished methods makes it important to complete propelled research here of irresistible sicknesses. This is going to be your best chance to achieve the biggest collection of members, conduct presentations, disseminate data, meet with potential scientists, trade learning and make an unmistakable imprint by fascinating developments at this event.
Neglected Tropical Diseases are the infectious diseases caused by organisms such as bacteria, viruses, protozoans, helminthes or parasites. These diseases may be caused due to the improper sanitation or hygiene. Tropical diseases basically emphasize on the pathogenesis of the various microorganisms and their therapeutic measures, coalesce of branches of microbiology especially clinical and diagnostic microbiology which deals with the cure and prevention of the tropical diseases. It represents an increasingly important cause of human morbidity and mortality throughout the world. Vaccine development is thus of great importance in terms of global health.
Target Audience-
- Academic Experts from Educational Institutes
- Microbiology Graduates and Post Graduates
- Research Guides and Scholars from microbiology
- Quality Analysts and Assurance guides
- Health Education Experts
- Healthcare Professionals
- Directors & Senior Directors
- Executive Directors Vice President
- Senior Vice Presidents
- Executive Vice Presidents and Heads
- Partners of CROs and CMOs
- Clinical Research organizations
- Pharma/Biotech and Medical Device industries
- Hospitals, Associations
- Scientists
- Industries & Healthcare sectors
Track 01: Emerging Neglected Tropical Diseases
Neglected tropical diseases are historically neglected at the community, national, and international levels and are endemic in many under-developed and developing countries. They affect populations living in poverty especially without proper sanitation and in close contact with various infectious vectors and disease causing livestocks and causes significant health and financial burdens across underdeveloped nations and widely impacts their socio-economic statuses. Neglected tropical diseases are caused by bacteria, virus, parasites, helminthes, protozoans etc. These including lymphatic filariasis, onchocerciasis, schistosomiasis, and soil-transmitted helminthiasis, represent a serious burden to public health. Unlike many public-health risks, such as malaria, tuberculosis, and HIV, the burden of human suffering caused by neglected tropical diseases remains poorly recognised by the global public-health community.
Track 02: Global NTD Epidemiology and Challenges
More than a billion people, about 1/6th of the world’s population, mostly in developing countries-are infected with one or more of the neglected tropical diseases (NTDs). Several national and international programs (e.g., the World Health Organization’s Global NTD Programs, the Centers for Disease Control and Prevention’s Global NTD Program, the United States Global Health Initiative, the United States Agency for International Development’s NTD Program, and others) are focusing on NTDs, to control or eliminate them. It is crucial to identify the risk factors of major NTDs, and describes the global burden of the diseases in terms of disability-adjusted life years (DALYs).
Track 03: Tropical Bacterial Diseases
The major (NTBDs) neglected tropical bacterial diseases are Cholera, Leprosy, Trachoma, Buruli ulcer. Buruli ulcer and Leprosy are caused by members of the Mycobacterium genus Mycobacterium leprosy and M. ulcerans and are responsible for most severe medical impact in the tropics and sub tropics. Trachoma is the result of infection of the eye with Chlamydia trachomatis and it is responsible for the visual impairment of about 1.8 million people, of whom 0.5 million are irreversibly blind. The dangerous infected disease is Buruli ulcer which is caused by Mycobacterium ulcerans. The early stage of the infection is characterised by a painless nodule or area of swelling. This nodule can turn into an ulcer after some days. Buruli ulcers most commonly affect the arms or legs but here fever is uncommon. Leprosy is another bacterial infectious disease caused by Mycobacterium leprae. This is also known as Hansen's disease (HD). The symptoms for this disease is that they develop include granulomas of the nerves, respiratory track, skin, and eyes.
Track 04: Tropical Viral Diseases
Tropical Viral infections include chikungunia, dengue, rabies etc. Chikungunya is transmitted to humans by infected Aedes albopictus and Aedes aegypti mosquitoes causing fever and severe joint pains. Other symptoms of chikungunya include fatigue disorder, headache, muscle pain, nausea, and rash etc. The disease shares its clinical symptoms with dengue and zika, and hence can be misdiagnosed in endemic areas. There is no cure for the disease and the treatment is focused only on relieving the symptoms. The virus is transmitted through the bites of infected female mosquitoes. Dengue fever is a mosquito- borne disease caused by the dengue virus. Symptoms begin 3-14 days after infection and include headache, high fever, muscle pain and joint pains, characteristic skin rash, and vomiting. Recovery generally takes about two to seven days.
Track 05: Tropical Protozoan Diseases
The infectious diseases that are caused by protozoa include Chagas diseases, Human African Tripanosomiasis, and Leishmaniasis, among others. Chagas disease is a tropical parasitic disease caused by the Protist, Trypanosoma cruzi which spreads through insects like “kissing bugs”. The symptoms of this disease changes generally over the course of the infection. In the early stage, symptoms are typically either present or mildly present and include fever, headaches, swollen lymph nodes, and local swelling at the bite injury. Leishmania parasites cause Leishmaniasis through the bites of sandflies. The disease is infected in 3 ways - cutaneous leishmaniasis, mucocutaneous leishmaniasis, and visceral leishmaniasis. The cutaneous form leads to skin ulcers while the mucocutaneous forms ulcers on the skin, nose and mouth .The visceral form starts with skin ulcers and then later progresses to enlarged spleen and liver, fever, and low red blood cells. There is a dire need of new drugs for tropical protozoan diseases which causes about 120,000 fatalities annually. Pentamidine, a broad- spectrum antiparasitic drug has been used for decades against several Trypanosomatids.
Track 06: Tropical Parasitic Diseases
Tropical Parasitic Diseases include Cysticercosis, Echinococcosis, lymphatic filariasis, and Sthistosomiasis among many others. Cysticercosis is characterized by tissue infection and caused by tapeworm. People infected with it have few or no symptoms for months but in some cases solid lumps of about 1-2 cms may develop under the skin, which gradually become painful and swollen. Echinococcosis is is also caused by tapeworm and are of 2 types- cystic echinococcosis and alveolar echinococcosis. The disease often starts without symptoms lasts for several months to years .The symptoms and signs that occur depend on the cyst's location and size in the body. Sthistosomiasis is commonly known as snail fever which is caused by parasitic flat worms, called sthistosomes. In this case the urinary tracks or intestines are infected. The symptoms include abdominal pain, bloody stool and blood in the urine and diarrhea; followed by kidney failure, bladder cancer and liver damage in the later stages. Lymphatic filariasis affects lymaphatic systems and leads to the enlargement of lymph nodes.
Track 07: Tropical Zoonotic Diseases
Zoonoses are the disease transmission between animals and humans through agents, which include bacteria, fungi, parasites, virus, or any other disease causing agents. About 1415 pathogens are known to infect humans and 62% of all infectious human pathogens are zoonotic which represent 76% of all emerging pathogens in the past decade. Except for the newly emerging zoonoses which have caused pandemic in the previous years, like SARS and H5N1, the others are not prioritized by national and international health systems and are therefore labelled into neglected tropical diseases. The diseases included in the zoonotic NTDs are anthrax, bovine tuberculosis, brucellosis, cysticercosis, human African trypanosomiasis, leishmaniasis and rabies.
Track 8: Rare Diseases
A rare disease affects less than 1:2000 of the entire general population. There are about 8,000 known rare diseases which are present throughout a person’s life due to lack of treatment options. Rare diseases are considered to be genetic and are asymptomatic for many and appears early in the life. The rarest of the rare diseases has been diagnosed only in 1 person which is ribose-5-phosphate isomerase deficiency. The categorization of rare diseases varies geographically. A disease that is rare in one geographic location might be endemic to another region. For e.g. cystic fibrosis is endemic to Europe but rare in Asia and South East Asia. In Finland, about 40 diseases are known as Finnish heritage disease since they have much higher prevalence only in Finland.
Since there is no huge pharmacy market for rare diseases, the drugs used to treat rare diseases are known as orphan drugs.
Track 9: Orphan Drugs
Drugs and biologics intended to treat rare and neglected diseases have been given the name, ‘ Orphan Drugs’ by the Orphan drug designation program for the safe and effective treatment and proper diagnosis or prevention of infection of rare diseases that affect 1:20000 people but are not expected to recover the costs of developing and marketing a treatment drug. In addition to orphan drugs, there are orphan vaccines for disease control and the prevention of spread of contagious rare diseases. Vaccines are expensive to develop for a small number of rare infectious diseases and hence only eight vaccines have been registered with the orphan status. Some of the Orphan drugs are, Rituximab, Bortezomib, Sorafenib, Sacrosidase, Clofezimine, and Nilotinib, etc. The nature of Orphan Drugs can create a difference in the amount of safety information for approval needed for limited number of patients in clinical trials and quality of the clinical trials.
Track 10: NTD in Clinical Research
The Pharmaceutical technology and development has historically neglected the infectious diseases that mainly or exclusively affect poor communities generally in low or middle income countries. Recently, collaborative clinical research studies addressing health needs of these low and middle income countries has become more frequent regarding therapeutic and diagnosis methods for neglected tropical diseases and is often conducted by non-commercial groups. The Good Clinical Practices codes (GCP) standardized by WHO provide global applicable standards for design, conduct, record, and reporting clinical trials. The Good Clinical Laboratory Practices (GCLP) codes are set by United Nations Development, World Bank, and WHO for Research and Training in Tropical Diseases. There are various challenges that need to be overcome for the improved diagnostics and management of the neglected tropical diseases.
- Binary Thinking and Syndromic Management of NTDS
- Implementing Research Compliant with Good Clinical Practice (GCP)
- Good Clinical Laboratory Practice (GCLP)
- Maintaining Improved Patient Care after Clinical Studies Have Come to an End
Track 11: Vaccines for Tropical diseases
A vaccine is a suspension of whole or fractionated bacteria or viruses that are rendered non-pathogenic. Vaccination has been extremely effective in preventing various serious infections that were once fatal and now have been eliminated. However, these infections still occur in parts of the under-developed and developing nations. Vaccines are frequently unavailable in developing countries. Each year, millions of people die from drug-treatable vaccine-preventable diseases. Furthermore, successful vaccines have yet to be developed for major global diseases such as tuberculosis. In addition, technologies that are used to develop and manufacture vaccines are often outdated and are not easily adaptable for rapidly responding to disease outbreaks, such as influenza.
- Hookworm vaccines
- Schistosomiasis vaccines
- Cysticercosis vaccines
- Echinococcosis vaccines
- Enteric protozoa vaccines
- Vaccines for leishmaniasis
- Anthelminthic Vaccines
Track 12: POC Treatment in NTD
POC diagnostics delivers rapid information for patient care. The common platform is the lateral flow immunoassay. Recently, emerging molecular diagnostics have met requirements for speed, low cost, and ease of use for POC applications. A major driver for POC development is the ability to diagnose infectious diseases at sites with a limited infrastructure. The potential use in both wealthy and resource-limited settings has fuelled an intense effort to build on existing technologies and to generate new technologies for the diagnosis of a broad spectrum of infectious diseases. POC diagnostics also reduce the reliance on presumptive treatment and thereby facilitate antibiotic control. Rapid diagnostic tests work by detecting analyte that are found in or extracted from clinical samples. There are two primary types of analytes: microbial antigens and patient antibodies that are specific for microbial antigens. However, there are emerging molecular technologies that enable nucleic acid-based approaches at the POC.
Track 13: Water, Sanitation and Hygiene
A proper water, sanitation and hygiene is crucial for preventing the cause of neglected tropical diseases, which affect over 1 billion people of lower socio-economic societies like rural areas since they have improper water facilities sanitation and hygiene facilities. Water is a fundamental human right. This provides access to safe water is one of the most effective instruments in promoting health and reducing poverty. Safely managed sanitation and safe wastewater treatment and reuse of water are fundamental to protect public health. WHO is giving efforts just to monitor the global burden of sanitation related disease and access to safely managed sanitation and safely treated wastewater development agenda. WHO also monitors the factors that enable or delay progress towards these targets. Proper sanitation is needed for prevention of many diseases including diarrhea, intestinal worms, trachoma which affects millions of peoples worldwide. Ensuring access to proper sanitation in households and educational and health-care and miscellaneous institutions is vital in reducing disease, improving nutritional outcomes, enhancing safety, well-being and educational prospects, especially for women and girls.
Track 14: Socio-economic impact of NTD
Neglected Tropical Diseases are not only responsible for the decrease in health and life expectancy, but also leads to dire economic consequences. The 5 prevalent NTDs are lymphatic filariasis, onchocerciasis, schistosomiasis, soil-transmitted helminths (ascariasis, trichuriasis, and hookworm infection) and trachoma. Studies reveal that over 40% of the population that currently lives in the tropics have high potential for NTD. The factors that cause high prevalence of NTDs include ecology, environmental factors, and lack of adequate public health efforts. Poverty also plays a strong role in the prevalence of NTDs, specifically by its social expression like substandard housing conditions, lack of access to safe and hygiene water, and poor environmental sanitation. A major determinant of risk for NTD transmission is poor housing which can obstruct and complicate vector control efforts, leading to increased exposure to diseases such as dengue, chagas disease, leishmaniasis, and lymphatic filariasis. Poor sanitation due to inadequate garbage disposal/collection can also result in breeding sites for many vectors which may result of spreading infectious diseases.
Track 15: Current advancements in NTD
Vaccines for neglected tropical diseases have been advanced into clinical research, product development and vaccine maintenance has become critical activities for the success of these vaccines. A new generation of vaccines for the neglected tropical diseases (NTDs) has now been introduced into clinical development, with the Na-GST-1/Alhydrogel Hookworm Vaccine already being tested in healthy adults. Necator americanus glutathione-S-transferase-1 (Na-GST-1) is a 24-kDa recombinant protein from N. americanus expressed in Pichia pastoris and purified by three chromatographic steps. This Clinical drug was formulated at a concentration of 0.1 mg/mL Na-GST-1 with 0.8 mg/mL of Alhydrogel in a glucose/imidazole buffer (10% dextrose, 10mM imidazole, pH 7.4). The drug product (vaccine) was produced according to current GMP and stored in temperature monitored refrigerators at 2–8°C. Other vaccines include nifurtimox-eflornithine combination therapy, benznidazole and nifurtimox. liposomal amphotericin B, paromomycin, and miltefosine, Anthelminthic Vaccines, Kinetoplastid Vaccines and therapeutic Chagas disease vaccine is also being developed by the Sabin PDP in collaboration with the Carlos Slim Foundation.
Track 16: Anti-Microbial resistance in NTD
Antimicrobial resistance threatens the efficacy and treatment of infections caused by infectious microorganisms and is one of the deadly and serious threats plaguing the health sectors and requires prompt action from government, society and private institutions. Since most infectious microorganisms have developed antibiotic resistance, a response against them is crucial as without effective antibiotics, the prognosis and treatments, especially antimicrobial chemotherapy will be rendered ineffective. According to statistics, in the year 2016, about 490,000 people globally developed multi-drug resistant TB.
Track 17: Animal Diseases
Diseases of animals remain a concern principally because of the economic losses they cause and the possible transmission of the causative agents to humans. The branch of medicine called veterinary medicine deals with the study, prevention, and treatment of diseases not only in domesticated animals but also in wild animals and in animals used in scientific research. The prevention, control, and eradication of diseases of economically important animals are agricultural concerns. Programs for the control of diseases communicable from animals to man, called zoonoses, especially those in pets and in wildlife, are closely related to human health. Further, the diseases of animals are of increasing importance, for a primary public-health problem throughout the world is animal-protein deficiency in the diet of humans. Indeed, both the United Nations Food and Agricultural Organization (FAO) and the World Health Organization (WHO) have been attempting to solve the problem of protein deficits in a world whose human population is rapidly expanding.
Tropical diseases are diseases that occur in tropical and subtropical regions. The diseases are less prevalent in temperate climates, due in part to the occurrence of a cold season, which controls the insect population by forcing hibernation. They are also called "neglected tropical diseases," because they generally afflict the world's poor and historically have not received as much attention as other diseases. However, many were also present in northern Europe and northern America in the 17th and 18th centuries before modern understanding of disease causation.
Tropical diseases are the infectious diseases that thrive in the hot and humid climatic conditions, which is suitable for the growth of micro-organisms like parasites, fungi, bacteria and virus. The population of vectors like mosquitos and insects also thrive which transmit disease pathogens. A large number of lives can be saved if they are diagnosed early and medical interventions are taken accordingly. The major factorial entities supporting the growth in demand for tropical disease diagnostic market are rise in population of tropical countries, increasing prevalence rate of neglected tropical diseases, access to healthcare services and government intervention. Due to high population rate, poverty, lack of sanitation and potable water the tropical disease has a high prevalence and incident rate in the tropical countries. Increasing prevalence of neglected tropical diseases like Chagas disease, Schistosomiasis are as a result of living in close contact with infectious vectors, domestic animals, and livestock.
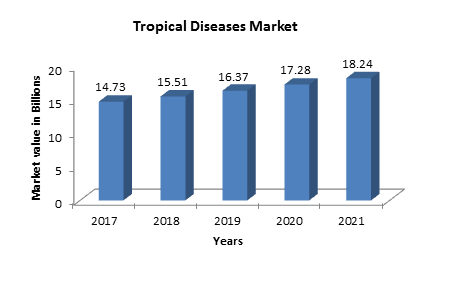
The global tropical infectious disease valued at $14.73 Billion in 2017 and is stipulated to reach $19.35 Billion by 2022 growing at a CAGR of 5.6%. The market growth of tropical infectious diseases is due to increase in the awareness of infections and their environmental factors, global prevalence of diseases, and increasing preference of point-of-care testing, and availability of funds for research and market is currently diagnostics.
Major Infection Prevention Research Associations around the Globe
- Asia Pacific Society of Infection Control
- British HIV Association
- British Infection Association
- Centers for Disease Control and Prevention
- European Centre for Disease Prevention and Control
- European Society for Clinical Microbiology and Infectious Diseases
- Health Protection Scotland
- Healthcare Infection Society
- Infection Control Association
- Infection Prevention & Control - American Nurses Association
- Infection Prevention Society
- Infectious Disease Society of America
- International Federation of Infection Control
- Royal Society for Public Health
- Society for General Microbiology
- The Infection Control Nurses Association
- The Royal Society of Tropical Medicine and Hygiene
- The Society of Health care Epidemiology of America
- UK Clinical Virology Network
- World Health Organization
Major Companies Associated with Infection Prevention Research
- Abbott Laboratories, UK
- Actavis, USA
- Aegerion Pharmaceuticals, Japan
- Alexion Pharmaceuticals Inc, Switzerland
- Almirall, Spain
- Amgen, USA
- Amicus Therapeutics, USA
- Amphastar Pharmaceuticals, Inc
- Araim Pharmaceuticals
- Astellas Pharma US
- AstraZeneca, Switzerland
- AstraZeneca, UK
- Baxter International Deerfield
- Bayer HealthCare, Germany
- Beacon Pharmaceuticals, Bangladesh
- Biotie Therapies Corp, Finland
- Bioxyne Limited, Australia
- Boehringer Ingelheim, Germany
- Celgene, Switzerland
- Chiesi Pharmaceutical, Italy
- Cohero Health, USA
- Daiichi Sankyo, Japan
- Dohmen Life Science
- Forest Laboratories, USA
- Gecko Health, USA
- Generics (UK) Ltd, UK
- Genus Oncology Vernon Hills, USA
- Genzyme, USA
- Gilead sciences, USA
- GlaxoSmithKline, UK
- Hormosan Pharma, Germany
- Ikris Pharma Network Pvt Ltd, India
- Kissei Pharmaceutical Co., Ltd, Japan
- Kyowa Hakko Kirin Co. Ltd, Japan
- Lallemand Pharma, Switzerland
- Marathon Pharmaceuticals
- Merck & Co, USA
- Millennium Pharmaceuticals
- Napp Pharmaceuticals Ltd, UK
- Novartis, Switzerland
- NPS Pharmaceuticals
- Octapharma, USA
- Onyx Pharmaceuticals, USA
- Otsuka Holdings Co., Ltd, Japan
- Panmira Pharmaceuticals, LLC, USA
- Pearl Therapeutics, Inc
- Pfizer, USA
- PharmaMar, USA
- Prosensa, Netherlands
- PT Boehringer Ingelheim, Indonesia
- Queensland Respiratory Laboratory Pty. Ltd, Australia
- Ranbaxy Laboratories Limited
- Raptor Therapeutics
- Roche, Switzerland
- Sanofi, France
- Sarepta Therapeutics, USA
- Sigma-Tau Pharmaceuticals, Italy
- Sunovion Pharmaceuticals, USA
- Swedish Orphan Biovitrum AB, Sweden
- Takeda, Japan
- TriStem Corp Ltd, UK
- ViroPharma
- Yungjin Pharm Ind. Co., Ltd, South Korea
Read More...
Conference Highlights
- Emerging Neglected Tropical Diseases
- Global NTD Epidemiology and Challenges
- Tropical Bacterial Diseases
- Tropical Viral Diseases
- Tropical Protozoan Diseases
- Tropical Parasitic Diseases
- Tropical Zoonotic Diseases
- Rare Diseases
- Orphan Drugs
- Neglected Tropical Diseases in Clinical Research
- Vaccines for Tropical Diseases
- POC Treatment in NTD
- Water, Sanitation and Hygiene
- Socio-economic impact of NTD
- Current Advancements in NTD
- Anti-Microbial Resistance in NTDs
- Animal Diseases
To share your views and research, please click here to register for the Conference.
To Collaborate Scientific Professionals around the World
| Conference Date | December 5-6, 2018 | ||
| Sponsors & Exhibitors |
|
||
| Speaker Opportunity Closed | Day 1 | Day 2 | |
| Poster Opportunity Closed | Click Here to View | ||
Useful Links
Special Issues
All accepted abstracts will be published in respective Our International Journals.
- Journal of Tropical Diseases & Public Health
- Tropical Medicine & Surgery
- Journal of Infectious Diseases & Preventive Medicine
Abstracts will be provided with Digital Object Identifier by